Here to Help You Change Your Life
We understand that making sure you know what to expect from your joint replacement experience is important to you. As you are reading through this material, if you have additional questions please reach out to us to discuss.
Each patient is unique, and can experience joint pain for different reasons. It’s important to talk to us about the reason for your joint pain so you can understand the treatment options available to you. Pain from arthritis and joint degeneration can be constant or come and go, occur with movement or after a period of rest, or be located in one spot or many parts of the body. It is common for patients to try medication and other conservative treatments to treat their hip or knee pain.
If you haven’t experienced adequate relief with those treatment options, you may be a candidate for Mako Total Hip, Total Knee or Partial Knee replacement, which may provide you with relief from your joint pain.
Mako SmartRobotics™, is a smart solution for joint pain, where
surgeons see more, and you keep more.
By guiding your doctor during surgery, Mako’s AccuStop™ technology allows your surgeon to cut less by cutting precisely what’s planned to help protect your healthy bone.
Mako SmartRobotics™ gets you back to the things you love, quicker.
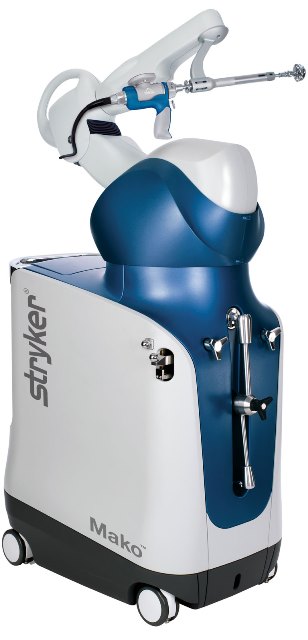
Mako SmartRobotics Assisted Technology
If you’re one of the millions of Americans suffering from pain caused by arthritis or an injury to the hip or knee, and you haven’t experienced adequate relief with conservative treatment options, Mako Robotic-Arm Assisted Surgery might be right for you.
Benefits of the Mako Robotic-Arm Assisted Replacement Surgery
- Surgeons are able to execute their surgical plans more accurately*
- Less likelihood of hip dislocation.
- Replication of the feeling of a natural hip.
- The soft tissue and ligaments around the joint are more protected from damage.*
- Preservation of healthy bone.
- Reduced blood loss.
- Shorter hospital stay.
- Mako patients surveyed 6 months after surgery reported lower pain scores than those who received a conventional joint replacement.
*In laboratory and clinical studies, and in comparison to conventional joint replacement surgeries
PLAN | Personalized surgical plan
The first step is patient-specific surgical planning. Before surgery, a CT scan of your joint is taken to develop a 3D virtual model of your unique joint. The 3D model helps your doctor see things he or she can’t typically see with an x-ray alone. Your doctor uses this model to evaluate your bone structure, disease severity, joint alignment and even the surrounding bone and tissue, so they can determine the optimal size, placement and alignment of your implant.
ASSESS | Range-of-motion assessment
Throughout your procedure, Mako provides real-time data to your surgeon. This allows them to continuously assess the movement and tension of your new joint, and adjust your surgical plan if desired.
PREPARE | Arthritic bone removal
In the operating room, your surgeon guides Mako’s robotic arm to remove the arthritic bone and cartilage from the joint. A virtual boundary provides tactile resistance to help the surgeon stay within the boundaries defined in your surgical plan.
INSERT | Implant placement
As the surgeon prepares to place the implant into its final position, the robotic-arm guides the implant at the desired angle defined in the surgical plan. This helps ensure the placement and alignment of the implant are performed according to plan.
It’s important to understand that the surgery is performed by an orthopaedic surgeon, who guides the robotic-arm during the surgery to position the implant in the knee and hip joints. The Mako Robotic-Arm does not perform surgery, make decisions on its own, or move without the surgeon guiding it. The Mako System also allows your surgeon to make adjustments to your plan during surgery as needed.
Hear from Our Patients

Testimonial 1: Robert Young
Making an Iron Man With Robotic-Assisted Knee Replacement Surgery

This revolutionary procedure put firefighter and scuba rescue diver Robert Young back in action.
By Laurie Yarnell
Knee pain forced him to give up rowing. Next was bowling. But “the straw that broke the camel’s back,” says Robert Young of Sloatsburg, was severe pain after he moved some tree trunks around his property in a wheelbarrow.
Young, 65, leads an active life. His job as a condominium superintendent keeps him on the move all day, climbing ladders, fixing elevators and the like. For 38 years, he’s been a volunteer firefighter; for the last five, he’s served the department as a scuba rescue diver.
But Young’s knee pain was interfering with activities he loved. Despite his “very high tolerance for pain,” he knew he had to do something about his knees. In the fall of 2016, Young consulted orthopaedic surgeon Arup Bhadra, MD, Director of the Total Joint Replacement Center at Good Samaritan Hospital, a member of the Westchester Medical Center Health Network (WMCHealth). After an exam and X-rays, Dr. Bhadra diagnosed Young with osteoarthritis (OA) in both knees.
Experienced by about 27 million Americans, OA is the most common chronic condition of the joints. Unlike in normal joints, where cartilage is a cushion between bones, in OA, cartilage breaks down, resulting in pain, swelling and decreased mobility. While OA is most commonly seen in those over 65, obesity, overuse, previous injury and genetics are contributing factors.
Given the deterioration of Young’s knees, replacements were recommended. Because he was on the younger side, in excellent shape and has good bone density, less-invasive partial replacements were recommended, says Dr. Bhadra. “Because partial replacements avoid the cutting of ligaments and muscles, you have a smaller incision and faster recovery.”
Damaged tissue and bone are replaced with a prosthetic implant. “We take a very thin slice of arthritic bone from the knee, and we add in metal pieces of the same shape, with a little plastic spacer in between, which works like smooth cartilage,” says Dr. Bhadra. In September 2016, he performed this procedure on Young’s left knee. Young recovered quickly, returning to light-work duty after five weeks and to the fire department after two months.
Young was so pleased that he returned to The Total Joint Replacement Center to have a partial replacement on his right knee in October 2017. This time, Dr. Bhadra offered him a newer, more technically advanced procedure — MAKO robotic-arm-assisted surgery. The Center started offering robotic surgery earlier that year, and Good Samaritan Hospital is one of the only hospitals in the region with this capability. “By bringing this option to Good Samaritan Hospital, we’re staying ahead of the curve and offering our patients the very best care,” says Dr. Bhadra.
“We call it robotic, but it’s actually minimally invasive, computer-assisted surgery,” says Dr. Bhadra. “The surgeon remains totally in control.” A robotic CT scan of the joint, taken before surgery, gives a three-dimensional picture of the joint.
During robotic-assisted surgery, he adds, “Technology helps enable the surgeon to be 100 percent precise, working almost like a GPS signal.” Less soft-tissue invasion also may result in quicker recovery, adds Dr. Bhadra.
“My mobility came back twice as fast the second time around with the robotic surgery,” Young confirms. “I got off painkillers earlier and had an easier and faster recovery.”
Indeed, just three weeks after his second surgery, Young was dancing at a reunion party held for the hospital’s joint-replacement patients and medical staff.
“The hospital was excellent, and Dr. Bhadra was amazing and very clear in explaining what was going to happen,” says Young.
Today, Young is back to his active routine and feels “wonderful – I’m 99 percent better.” In fact, his ability to keep up with his 30-year-old buddies at the firehouse has earned him a new nickname: Iron Man.
Important Information
Hip & knee replacements Hip joint replacement is intended for use in individuals with joint disease resulting from degenerative and rheumatoid arthritis, avascular necrosis, fracture of the neck of the femur or functional deformity of the hip. Knee joint replacement is intended for use in individuals with joint disease resulting from degenerative, rheumatoid and post-traumatic arthritis, and for moderate deformity of the knee.
Joint replacement surgery is not appropriate for patients with certain types of infections, any mental or neuromuscular disorder which would create an unacceptable risk of prosthesis instability, prosthesis fixation failure or complications in postoperative care, compromised bone stock, skeletal immaturity, severe instability of the joint, or excessive body weight.
Like any surgery, joint replacement surgery has serious risks which include, but are not limited to, pain, bone fracture, change in the treated leg length (hip), joint stiffness, hip joint fusion, amputation, peripheral neuropathies (nerve damage), circulatory compromise (including deep vein thrombosis (blood clots in the legs)), genitourinary disorders (including kidney failure), gastrointestinal disorders (including paralytic ileus (loss of intestinal digestive movement)), vascular disorders (including thrombus (blood clots), blood loss, or changes in blood pressure or heart rhythm), bronchopulmonary disorders (including emboli, stroke or pneumonia), heart attack, and death.
Implant related risks which may lead to a revision of the implant include dislocation, loosening, fracture, nerve damage, heterotopic bone formation (abnormal bone growth in tissue), wear of the implant, metal sensitivity, soft tissue imbalance, osteolysis (localized progressive bone loss), audible sounds during motion, and reaction to particle debris.
The information presented is for educational purposes only. Speak to your doctor to decide if joint replacement surgery is appropriate for you. Individual results vary and not all patients will return to the same activity level. The lifetime of any joint replacement is limited and depends on several factors like patient weight and activity level. Your doctor will counsel you about strategies to potentially prolong the lifetime of the device, including avoiding high-impact activities, such as running, as well as maintaining a healthy weight. It is important to closely follow your physician’s instructions regarding post-surgery activity, treatment and follow-up care. Ask your doctor if a joint replacement is right for you.
Stryker Corporation or its other divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: Mako, Stryker, Triathlon. All other trademarks are trademarks of their respected owners or holders.
References:
Nawabi DH, Conditt MA, Ranawat AS, Dunbar NJ, Jones J, Banks SA, Padgett DE. Haptically guided robotic technology in total hip arthroplasty - a cadaver investigation. Proc Inst Mech Eng H. 2013 Mar22 7(3):302-9 Illgen R. Robotic assisted total hip arthroplasty improves accuracy and clinical outcome compared with manual technique. 44th Annual Advances in Arthroplasty Course. October 7-10, 2014, Cambridge, MA.F 1. Bell, Stuart W. MBChB, MRCP, FRCS(T&O), Anthony, IainPhD, Jones, Bryn MBChB, FRCS(T&O), MacLean, Angus MBChB, RCS(T&O), Rowe, Philip BSc(Hons), PhD, and Blyth, Mark MBChB, FRCS(T&O). Improved accuracy of component positioning with robotic-assisted unicompartmental knee arthroplasty. The Journal of Bone and Joint Surgery. Volume 98-A: Number 8. April 20, 2016. pp 627-35. Bell, Stuart W., Anthony, Iain, Jones, Bryn, MacLean, Angus, Rowe, Philip, and Blyth, Mark. Improved accuracy of component positioning with robotic-assisted unicompartmental knee arthroplasty. The Journal of Bone and Joint Surgery. Volume 98-A: Number 8. April 20, 2016. pp 627-35. Mistry J, Elmallah R, Chughtai M, Oktem M, Harwin S, Mont M. Long-Term Survivorship and Clinical Outcomes of a Single Radius Total Knee Arthroplasty. International XXVIII. Designed to maintain collateral ligament stability throughout the range of motion. Stryker-Initiated Dynamic Computer Simulations of Passive ROM and Oxford Rig Test, Stephen Piazza, 2003. Wang H, Simpson KJ, Ferrara MS, Chamnongkich S, Kinsey T, Mahoney, OM. Biomechanical differences exhibited during sit-to-stand between total knee arthroplasty designs of varying radii. J Arthroplasty. 2006;21(8):1193-1199. Gómez-Barrena E, Fernandez-García C, Fernandez- Bravo A, Cutillas-Ruiz R, Bermejo-Fernandez G. Functional performance with a single-radius femoral design total knee arthroplasty. Clin Ortho Relates Res. 2010;468(5):1214-1220. MKOHMT-PE-3_Rev-1_13841
Copyright © 2017 Stryker Corporati